Completing a discharge summary for an ICU patient is one of the most time-consuming documentation tasks a physician faces. For a complex patient with a 10–20 day ICU stay, reconstructing the full clinical narrative — vitals trends, medication changes, procedures, complications — from handwritten notes can take 2–3 hours.
In many hospitals, this burden is compounded. Doctors must produce documentation that satisfies not just hospital records requirements, but also the detailed criteria set by Third Party Administrators (TPA) for insurance claim processing.

The Documentation Burden in ICUs
ICU doctors face a unique double burden: high patient volumes and extensive medicolegal documentation requirements — simultaneously.
When a patient is discharged from the ICU, the attending doctor must produce a summary that covers:
- Complete admission history and diagnosis
- Day-by-day clinical course across the entire ICU stay
- All procedures performed (intubation, central line placement, dialysis, surgeries)
- Complete medication history including vasopressors, antibiotics, and sedation
- Severity scores (SOFA, APACHE) at admission and during the stay
- Complications encountered and how they were managed
- Final outcome — discharge condition or, in the case of death, cause and manner
This document is then submitted to TPA insurance companies for claim processing, to hospital management for records, and retained as medicolegal evidence in case of disputes.
Any gaps, inconsistencies, or incomplete documentation can result in delayed or rejected insurance claims — adding administrative burden at exactly the wrong time. In medicolegal proceedings, documentation gaps are interpreted unfavorably against the treating doctor.

The Traditional Process: Why It Fails
Most ICU doctors rely on a combination of handwritten bedside notes, memory, and printed laboratory reports to reconstruct the clinical course at the time of discharge.
This approach has several inherent problems:
Incomplete recall. For a 15-day ICU stay, a doctor cannot reliably recall every clinical decision, medication change, or procedure. Details get omitted.
Time pressure. Discharge summaries are often completed at the end of a shift or after the patient has already left. The doctor is typically already tired and managing new admissions.
Inconsistent formatting. Without a structured template, summaries vary widely in completeness. What one doctor includes in detail, another may summarize in a single sentence.
Medicolegal vulnerability. An incomplete or inconsistent discharge summary exposes the treating doctor to risk in legal proceedings. Documentation gaps are interpreted unfavorably.
The fundamental problem isn’t that doctors don’t know what to document — it’s that the traditional workflow forces them to document at the wrong time (discharge) from incomplete information (memory and scattered notes). The fix is upstream: structured data collection during the stay.
How AI-Assisted Documentation Changes Everything
Modern large language models — specifically Google Gemini — can read structured clinical data and generate comprehensive, coherent summaries that would take a doctor hours to write manually.
The key word is structured. The AI is only as good as the input it receives. This is where tools like Rivara Health’s ICU Summary Generator make the difference.
Instead of generating summaries from unstructured handwritten notes, the ICU Summary Generator collects structured clinical data throughout the patient’s stay:
- Admission details: demographics, diagnosis, comorbidities
- Daily notes: vitals, medications administered, procedures, SOFA score, clinical assessment
- Events: significant clinical events, changes in management, family counselling notes
- Outcome: discharge condition or cause of death
When the time comes to generate a summary, the AI has a complete, structured clinical timeline to work with. The result is not a guess — it is a coherent synthesis of everything that was documented.
What if your daily notes wrote the discharge summary for you?
Rivara Health collects structured data during the ICU stay and generates the full discharge summary automatically — in under 2 minutes.
What Makes a Good AI ICU Discharge Summary for TPA?
A TPA-ready discharge summary must satisfy specific documentation requirements. Rivara Health’s AI prompt is engineered to produce summaries that include all of the following elements:
1. Admission Diagnosis and Clinical Indication for ICU Admission
The summary must clearly state why the patient was admitted to the ICU, the primary diagnosis, and any relevant comorbidities. This establishes the medical necessity of the ICU stay — a key criterion for TPA approval.
2. Day-by-Day Clinical Course
TPA companies require a narrative of the clinical course, not just a snapshot of admission and discharge. The AI synthesizes the daily notes into a coherent clinical story: initial deterioration, response to treatment, complications, and recovery trajectory.
3. Procedures and Interventions
Every procedure must be documented: intubation, central venous catheter placement, arterial line monitoring, mechanical ventilation parameters, dialysis sessions, blood transfusions, surgical interventions. Each procedure adds to the complexity billing justification.
4. Medication Documentation
Complete medication history including antibiotics (with culture and sensitivity data where available), vasopressors, sedation, anticoagulants, and all other significant drugs. Duration of each agent and rationale for changes must be included.
5. SOFA Score Documentation
The Sequential Organ Failure Assessment (SOFA) score provides an objective measure of ICU illness severity. TPA companies and courts both use SOFA scores to assess whether the level of ICU care provided was justified. Rivara Health’s ICU Summary Generator automatically calculates and tracks SOFA scores daily across all 6 organ systems.
For a deep dive into SOFA scoring, reference ranges, and documentation best practices, see our complete SOFA score guide for ICU clinicians.
6. Complications and Management
Any complications that arose during the ICU stay — hospital-acquired infections, ventilator-associated pneumonia, acute kidney injury, arrhythmias — must be documented along with the management taken.
7. Outcome
For discharge: condition at discharge, instructions, follow-up plan. For death: time of death, immediate cause, underlying cause, and whether family was counselled.
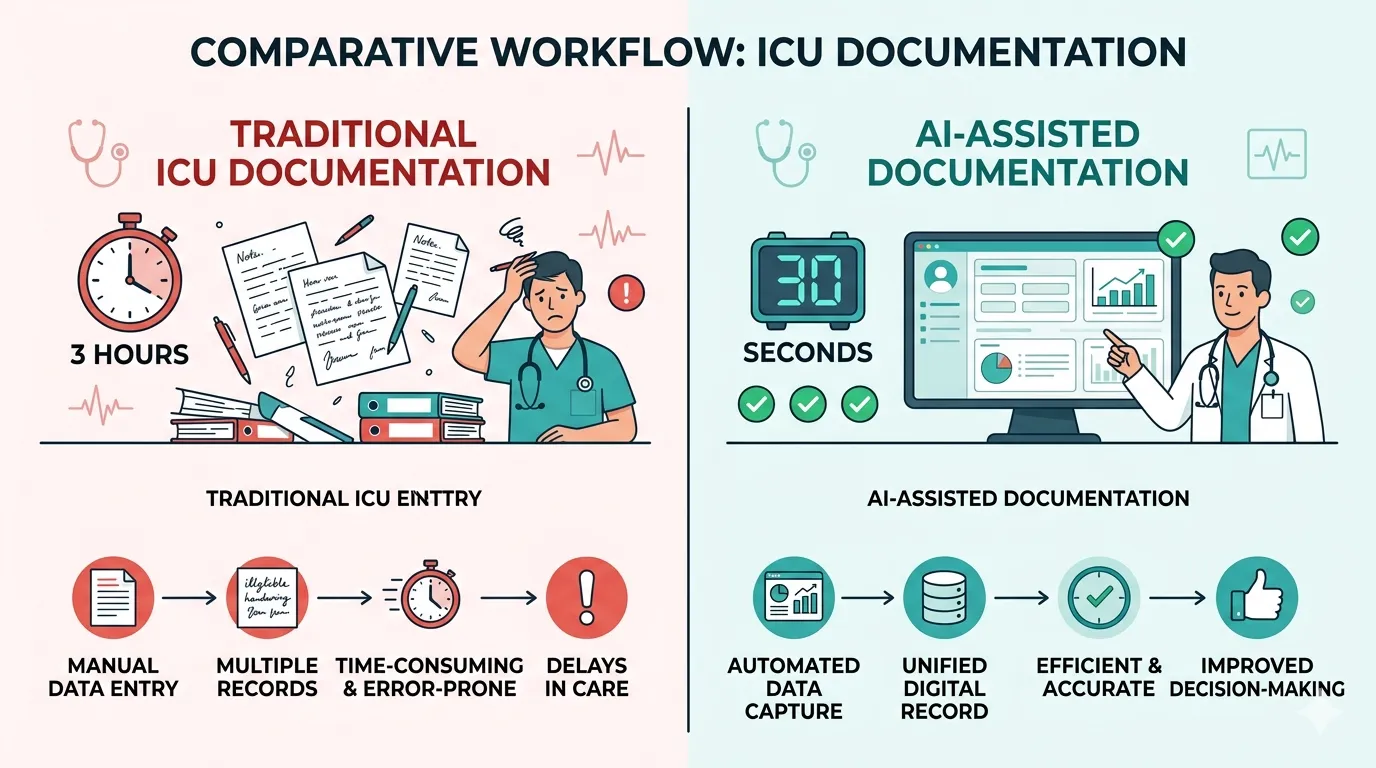
The Result: 3 Hours to 2 Minutes
With Rivara Health’s ICU Summary Generator, what used to take 2–3 hours of manual documentation now takes under 2 minutes.
Doctors log structured daily notes throughout the patient’s stay — which takes only 3–5 minutes per day as part of the existing ward round workflow. When it is time to generate the discharge or death summary, the AI has a complete, structured clinical dataset to synthesize.
The generated summary is reviewed by the doctor, adjusted if needed, and exported as a formatted PDF — ready for TPA submission.
Your patients deserve documentation that protects them — and you
Generate complete, medicolegal-grade ICU discharge summaries with daily SOFA scores, vasopressor records, and structured clinical narratives. Free to use.
Beyond Speed: Medicolegal Quality
The quality of AI-generated documentation is not just about speed. Structured, consistent documentation is inherently safer from a medicolegal standpoint.
Every entry in the ICU Summary Generator is timestamped and append-only. No entry can be modified after the fact — only new entries can be added. This creates a tamper-evident audit trail that holds up in legal proceedings.
This is the same principle used in aviation black boxes and banking transaction logs: an immutable record that reflects what was done, when, and by whom. In medicolegal disputes, this level of documentation integrity can be decisive.
Getting Started
Rivara Health’s ICU Summary Generator is free to use. No installation is required — it runs entirely in the browser. Doctors can begin admitting patients and logging notes immediately.
The ICU Discharge Summary Generator is available now. For a complete guide to getting the most from the tool, including how to structure daily notes for the best AI output, see our guide to SOFA score documentation and ICU discharge best practices.
Related reading: ICU Discharge Summary for TPA Insurance Claims: A Complete Guide
Medical Disclaimer
This article is for informational and educational purposes only. It does not constitute medical advice, diagnosis, or treatment. Always consult a qualified healthcare professional for clinical decision-making. Rivara Health provides documentation tools — clinical judgement remains with the treating physician.
Reduce ICU Documentation Time by 90%
Generate medicolegal-grade ICU discharge summaries in under 2 minutes. Built for Indian hospitals, designed for TPA compliance.